A Weight-Loss Injection Causes A SHOCKING Medical Emergency | Casualty
The moment the ambulance crew eased through the doors, the mood inside Casualty changed—because the patient didn’t look like someone who was simply “under the weather.” He looked rattled. Worried. Like he’d been fighting something invisible for days and only now realised it had become an emergency.
In the resus bay, a team member leaned in close, voice steady, asking for updates—how he was doing, what had been happening, what had brought him in tonight. But before the questions could fully settle, you could feel the panic in the small details: the way he tried to get away from the situation, the way he hesitated like he didn’t want anyone to “make a fuss,” and the way he kept talking like he already expected the worst.
And then—almost immediately—the evidence started to show.
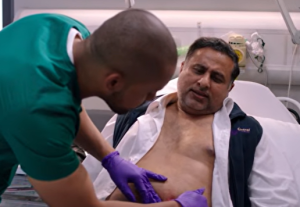
Someone took a closer look at his arm, scanning the injection site with that clinical focus that doesn’t miss a thing. The skin didn’t just look sore. It looked wrong. There was redness, irritation—concern rising fast as the team realised this wasn’t typical post-injection discomfort.
“This looks sore,” one of them said, but it wasn’t meant as reassurance. It was the kind of observation that turns into a diagnosis in real time. Another voice followed, more direct now: the injection site looked infected. Not minor. Not something to ignore.
The conversation moved quickly, like it always does when time matters.
“What have you been taking?”
He hesitated, then answered: Liracept. The name landed in the room like a warning. The staff exchanged glances—because they’d seen complications before, but never quite like this. The next question came sharper, as if they were trying to rule out a pattern: “Are you diabetic?”
“No,” he replied, too quickly, like he needed everyone to know it wasn’t that.
But the team wasn’t satisfied. Not yet.
The patient began to explain—familiar words, the kind that come up in emergency rooms across the country. He’d been overweight. He’d wanted help. The NHS criteria didn’t feel like they were going to work for him, so he’d gone elsewhere. He’d told himself he was doing what he had to do. He’d sat on his arse all day—he didn’t soften it, didn’t dress it up—and he’d worried he’d get sacked if he couldn’t shift the weight fast enough.
So he turned to the injection.
He said it like a success story at first. Like he was proud of what it had done for him. He’d heard it was a miracle drug, and he believed it. He’d lost seven stone. He’d done the work, followed the plan—at least, that’s what he thought.
Then a different voice cut in, challenging him with realism. “No such thing, mate.”
But he wouldn’t back down. Not now. Not after what he’d achieved. The debate lasted only seconds, because in medicine, you don’t argue long—you act. Even if his weight-loss journey had been successful, the injection site told a completely different story.
The team decided to move him onto antibiotics—because infection was the immediate danger, and delaying treatment could turn a bad situation into something far worse.
For a moment, it looked like they were in control again. Like the right steps were being taken. But the patient wasn’t just dealing with pain. His condition was progressing.
Nicole—sharp, observant, the kind of clinician who notices changes before they become alarms—checked his temperature and found it was still rising. She asked how he was feeling. His response wasn’t dramatic, but it was honest: rough. Like his body had been fighting something and losing ground.
Nicole confirmed what the patient already seemed to fear: yes, the rising temperature was likely the infection. But then she asked a second question—one that made everything more complicated.
“Is that why you got confused?”
Confused.
The word hit the room harder than it should have. Because confusion isn’t a symptom you see when things are stable. It’s what happens when the body is overwhelmed—when infection affects the brain, or when side effects begin to spiral.
And suddenly the patient’s story became messy, inconsistent—like he’d been trying to make sense of symptoms while they were happening.
He started to explain how he’d ended up going the wrong way down a diversion. Like his body hadn’t been fully cooperating. Like he’d been making decisions while his mind wasn’t clear.
Nicole didn’t dismiss it. She offered a chilling possibility: it might not be only the infection. It could also be the Liracept itself—its side effects, its dosing, the dangerous consequences of using it wrong.
The patient stared, confused